
Medical Bills: A Leading Cause of Bankruptcies in the US
Medical bankruptcies occur when consumers are forced to declare bankruptcy because of the cost of medical treatments. However, there is no single definition of “medical bankruptcy.”
In a 2009 study of all bankruptcies in 2007, researchers classified a “medical bankruptcy” as one where persons had mortgaged a home to pay medical bills, had medical bills greater than $1,000, or had lost at least two weeks of work due to illness. According to that definition, 62.1 percent of all bankruptcies in the United States were “medical bankruptcies.” A 2015 study by the Kaiser Family Foundation found that medical bills caused 1 million U.S. adults to declare bankruptcy every year and that 26 percent of Americans aged 18 to 64 struggled to pay medical bills. The most common cause of medical debt, according to this study, was an unexpected refusal by insurance companies to pay for a medical procedure. [1]

Filing for bankruptcy is often considered a worst-case scenario and for many Americans who do pursue that last-ditch effort to rescue their finances, it is because of one reason: healthcare costs. A study from academic researchers found that 66.5 percent of all bankruptcies were tied to medical issues, either because of high costs for adults with health care or time out of work. An estimated 530,000 families turn to bankruptcy each year because of medical issues and bills, the research found. Other reasons include unaffordable mortgages or foreclosure, at 45 percent; followed by spending or living beyond one’s means, 44.4 percent; providing help to friends or relatives, 28.4 percent; student loans, 25.4 percent; or divorce or separation, 24.4 percent. [2]
The cost of health care is a significant financial burden for many people. A 2021 Census Bureau study found nearly 1 in 5 households (19%) couldn’t pay for medical care when it was needed. The Consumer Financial Protection Bureau reported in 2022 that whenever debt collectors contacted consumers, medical debt was the most likely reason. This close connection between poor health and financial troubles carries through to bankruptcy. The link was notably made in a 2000 study that concluded medical bills accounted for 40% of bankruptcy filings the previous year.
That was years before the Affordable Care Act, but the expansion of health insurance coverage under the law known as Obamacare hasn’t seemed to make much difference. In a 2019 study of 910 Americans who filed for bankruptcy, two-thirds said their filings were tied to medical issues. [3] Figure 1
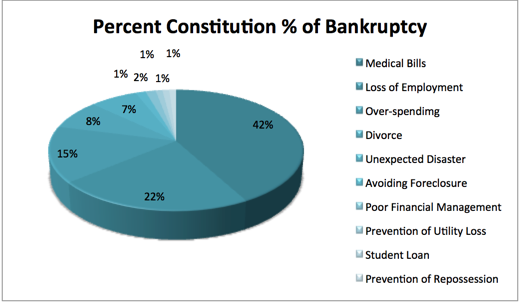
Figure 1: Bankruptcy Percentage
A study claims that over two million people are adversely affected by their medical expenses. [4]. National surveys confirm that medical bills frequently cause financial hardship, and the US Consumer Financial Protection Bureau reported that they were by far the most common cause of unpaid medical and dental bills sent to collection agencies in 2014, accounting for more than half of all such debts. Myriad anecdotes of a Nobel laureate who sold his medal to pay medical bills, or the more than 250 000 GoFundMe medical campaigns last year. [5Reports from different entities are constantly published, such as the survey results of people with employer-sponsored insurance by the Kaiser Family Foundation (KFF) / LA Times Survey in 2019. The study found that one in five people surveyed have been contacted by collection agencies, while 9% of those surveyed stated that they had declared personal bankruptcy due to medical expenses. [6]
A lot of people, a little over 60%, are filing bankruptcy at least in part because of medical or dental bills. Most of them are insured. It’s clear that despite health insurance, there are many, many people incurring costs not being covered by their insurance. Medical debt is incredibly common, it’s the main cause of calls from collection agencies, and the vast majority of people with it have insurance. One out of every six Americans has an unpaid medical or dental bill on their credit report, amounting to $81bn in health care debt owe nationwide, while about one in 12 Americans went without any medical insurance throughout 2018. Even as many Americans struggle to afford health insurance coverage in the first place, those that have it been not insulated from facing massive debt due to medical and dental bills. [7] Figure 2.
Figure 2: Medical Bill
As it turns out, medical bankruptcy is almost unheard of outside of the United States. Other developed economies (except China) have single-payer health care systems where medical costs are financed by taxes, not by premium-financed insurance. In these countries, there are no out-of-pocket costs for medical or dental care and thus no bankruptcy caused by medical debts. In countries without single-payer systems besides the United States, there is generally no requirement that medical procedures be provided without payment, and thus procedures are paid for prior to treatment being rendered. [1]
It is hard to tell what the actual impact of medical expenses is with so many different interpretations of study results. What is known is that there are many people who are so affected by healthcare debts that they need to file for bankruptcy. There are many reasons that people file for bankruptcy. Medical expenses do have an effect on people’s financial situations, causing some financially responsible people to file for bankruptcy. For others, the expenses are the final push over the financial cliff they were walking along. [8]
The debate over medical expense bankruptcy will continue to have a place on political platforms, around dinner tables, and in academia for the foreseeable future. Politicians will continue to spin the numbers to work for the votes they need. What is undeniable, however, is that a vast number of people are influenced by medical expenses to file for bankruptcy in America.
Naturopathic Medicine Can Help People to Avoid Bankruptcies
Naturopathic medicine is a complete alternative care system that uses a wide range of approaches such as nutrition, herbs, manipulation of the body, exercise, stress reduction, and acupuncture. Parts of naturopathy are sometimes used with conventional medicine as a complementary therapy. Naturopathic medicine is a holistic approach (meaning it is intended to treat the whole person) that tries to enlist the healing power of the body and nature to fight disease.
Supporters claim that naturopathic medicine uses the healing power of nature to maintain and restore health. Their goal is to create a healthy environment inside and outside the body. Supporters claim naturopathic medicine prevents illness because people are taught healthy diets and lifestyles to avoid disease. Treatment is focused on the cause of the disease, rather than on the symptoms. Naturopathic doctors may diagnose illness with many of the same methods used in conventional medicine. They use x-rays, laboratory tests, and physical exams to try to identify the problem. However, naturopathic treatment does not generally use drugs, radiation therapy, or major surgery. [9] Figure 3.

Figure 3: Bankrupt
Acceptance of Natural medicine due to its cost effectiveness
The increasing use of natural medicine has been driven, in part, by the growing prevalence of chronic disease that is associated with our ageing population: managing the pain and disability of chronic disease is one of the main reasons that Australians turn to natural medicine. This in turn has led to an increase in participation by private health insurers, as many offer rebates for natural medicine. This acceptance has stimulated growth in the natural medicine industry, which now generates total revenue of $4 billion and an annual growth of 3.1%, employing 35,230 people in 29,359 small businesses. Figure 4.
Figure 4: cost effectiveness of natural medicine
However, the wide public acceptance and use of natural medicine has raised concerns about the lack of evidence supporting many of the claims made about its effectiveness. In 2015 an Australian government review of health fund rebates for natural medicine in Australia investigated the effectiveness, cost-effectiveness, safety and quality of 17 natural therapies and reported that clear evidence for 17 natural therapies could not be found. The review focused on whole practice evidence, overlooking evidence for individual elements of those therapies. This review provoked a strong response from practitioners, researchers, and consumers in the natural medicine industry, who claimed that the review was hampered by the lack of evidence for the interventions and several methodological limitations. [26]
Naturopathy Is Typically Not Covered By Insurance
Naturopathic medicine uses many different techniques and methods. Practitioners act mostly as teachers. They decide how to treat a particular patient based on case history, observation, medical records, and previous experience. Naturopathic treatment can include nutritional medicine and fasting; herbs, minerals, and vitamins; homeopathy; Chinese medicine; manipulation of muscles, the spine, and other bones; acupuncture; counseling and hypnotherapy; massage; colonics (enemas); hydrotherapy, heat, and cold applications; therapeutic exercise; and some minor surgery.
Counseling or behavioral medicine is an important part of naturopathic medicine. Practitioners are usually trained in counseling, biofeedback, stress reduction, and other means to improve mental health. They may also use other unproven techniques such as ozone therapy for people with cancer and AIDS. These treatments have shown no benefit in curing cancer or other diseases. Figure 5.

Figure 5: Ozone Therapy
Treatment by naturopathic doctors is not covered by many insurance policies, including those offered through Medicare and Tricare. A few states require that treatment by licensed naturopathic doctors be covered by insurance companies. States that license naturopathic doctors as primary care providers may provide coverage on Medicaid programs. [9]
PGLBP Treatment by Acupuncture is Cost Effective
Pelvic girdle and low back pain (PGLBP) is common during pregnancy affecting 5 to 76% of pregnant women, depending on clinical definition. PGLBP is characterized by pain between the posterior iliac crest and the gluteal fold, particularly in the vicinity of the sacroiliac joints (SIJ) or in the lumbar region above the sacrum. PGLBP has a complex, multifactorial and incompletely understood pathophysiology. Strenuous work, previous low back or pelvic girdle pain and weight gain during pregnancy are risk factors. Pain increases with standing position and physical activity. Diagnosis relies on analyzing functional complaints and performing basic pain provocation tests. Symptoms tend to disappear after delivery but may continue up to 3 years in about 20% of women. Because it results in poor functional and quality of life scores, PGLP represents an economic burden, especially regarding indirect non-healthcare costs related to time lost for work and leisure. Figure 6.
Figure 6: Pelvic Girdle and Low back pain
As for treatment, European guidelines recommend individualized exercises focusing on stabilizing exercises, information and reassurance, and a limited choice of pain medications, with acetaminophen as first choice. Over 50%-75% of women with PGLBP receive little or no intervention from healthcare providers. There is some evidence of low back pain alleviation during pregnancy by acupuncture but offering acupuncture as part of routine obstetrical care would result in extra costs for the health system and patients. [10]
Acupuncture is Cost Effective in The Treatment of Chronic Back Pain
Acupuncture is increasingly used in patients with chronic pain, but there is a lack of evidence on the cost-benefit relationship of this treatment strategy. According to international cost-effectiveness threshold values, acupuncture is a cost-effective treatment strategy in patients with chronic neck pain. [11] Figure 7.
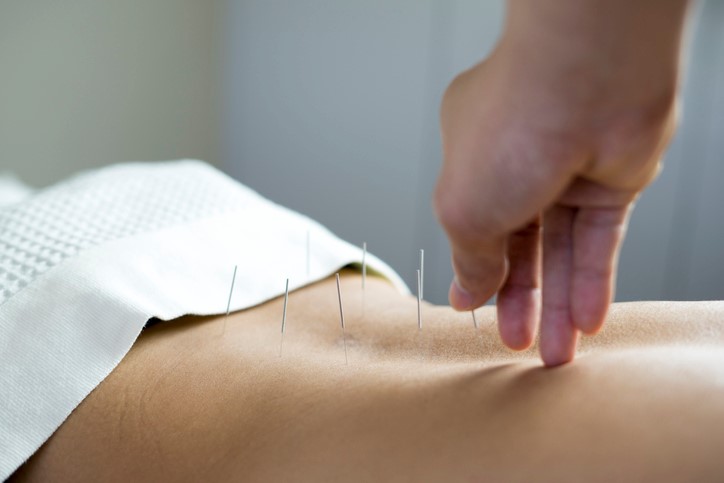
Figure 7: Acupuncture
Acupuncture Using a New Skin Stimulus Tool Called M-Test
Although every hemodialysis patient has multiple symptoms, many previous studies on the efficacy of acupuncture treatment for hemodialysis patients focused on their typical symptoms individually such as itchiness, fatigue, insomnia, and pain. However, a hemodialysis patient has a wide range of nonmotor symptoms such as itchiness, dizziness, and palpitations in addition to orthopedic pain including back pain. Acupuncture treatment can simultaneously reduce a wide range of dialysis patients’ symptoms; however, there have been few studies discussing the efficacy of acupuncture treatment focusing on all symptoms that a single patient suffers.
M-Test is a treatment approach to diagnose and treat patients by using a measure based on symptoms accompanied by body movements such as pain and dizziness. Its basic movements consist of simple movements that anyone can perform. By analyzing symptoms accompanied by movements, we can easily determine which meridians have problems and how they should be restored and what kind of treatments are required. M-Test is simple and safe and treats patients’ complaints effectively and quickly.
By simulating acupuncture points that are led by this method, many case studies show that a patient’s various symptoms get simultaneously relieved when the body movement gets improved. Multiple medicines are required to treat diverse symptoms of dialysis patients based on Western medicine. It is of a low cost and has a significant economic benefit to be able treat patients without medicine. Figure 8.

Figure 8: Acupuncture Points
In addition, needles have been mainly used as a stimulating tool in discussing efficacy of acupuncture treatment for dialysis patients. It is a safe treatment approach if conducted by trained acupuncturist; however, there are risks of increased susceptibility to infection due to their lower immunity as well as hemorrhage from use of an anticoagulant. Therefore, it is desirable to use a less invasive or noninvasive stimulation approach. [12]
Acupuncture in severe IBS
There is insufficient evidence to determine whether acupuncture is a cost-effective treatment for irritable bowel syndrome. Acupuncture as an adjunct to usual care is not a cost-effective option for the whole IBS population; however, it may be cost-effective for those with more severe irritable bowel syndrome. [13] Figure 9.
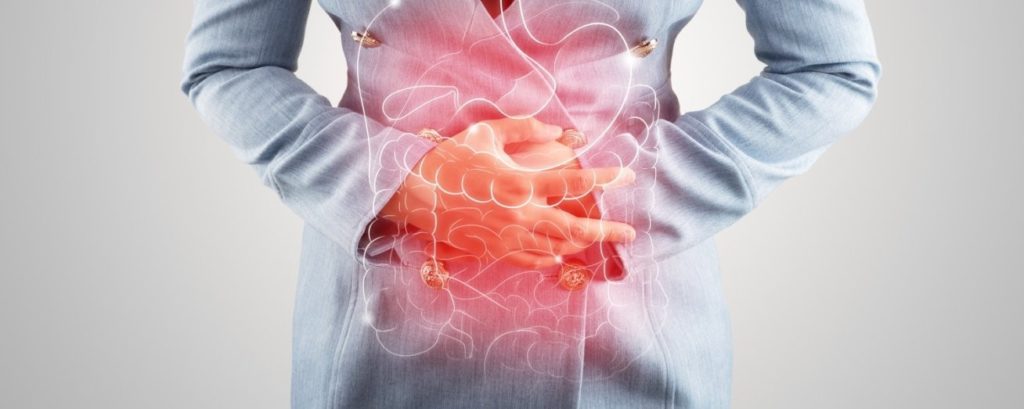
Figure 9: Acupuncture in IBS treatment
Alternative Medicine Cost Effectiveness by Alma-Ata Declaration
The Alma–Ata declaration recognized the value of traditional systems of medicine and advocated the integration of safe and effective traditional medicine practices into primary health care. The World Health Organization has urged its member states to integrate complementary and alternative medicine (CAM) into their national health care systems. The National Policy on Indian Systems of Medicine and Homoeopathy 2002 emphasized the need for a meaningful phased integration of the Indian Systems of Medicines with modern medicine. The government of India also has iterated that the Indian Systems of Medicine offers a wide range of preventive, promotive, and curative treatments that are cost-effective and efficacious. [14] Figure 10.

Figure 10: No to Private Health Care
Evidence suggests that a nation could save millions in health care costs and provide better quality of care without compromising patient outcomes if alternative medicine is widely practiced. Comprehensive systematic reviews have identified emerging evidence of the cost-effectiveness of various alternative therapies, compared to the usual care. [15]
Massage Therapy replace opioids
A study specifically examined the costs and benefits of replacing opioid pain killers with massage therapy in cases where evidence indicated this approach to be appropriate and effective. The President’s Council of Economic Advisors (CEA) estimated that in 2015, the economic cost of the opioid crisis was $504 billion. According to the Joint Commission nonpharmacologic approaches or techniques like massage therapy can replace opioids for many types of pain. The number of patients who could be treated either by massage therapy or opioid prescriptions was determined through analysis of data published by the Center for Medicare and Medicaid Services in a report for calendar year 2015. [16]
The number of individuals with the potential to benefit from massage therapy can be as many as 5 million patients in the U.S., with the potential to reduce the number of people with addiction disorder by 111,137 people per year. Figure 11.

Figure 11: Say no to Opioids
This projection suggests providing massage therapy as a tool for pain management instead of opioids could save the United States between $23.59 and $25.99 billion annually in social and economic costs associated with early death, treatment, and crime prevention. According to John Dunham of John Dunham & Associates which conducted the research and analysis, “The opioid addiction epidemic impacts real people in a way that not only harms their families but also leads to negative economic impacts. This analysis uses reasonable and moderate assumptions, as well as the best data available from both government and academic sources to calculate that incorporating massage therapy into pain management practices would not only be cost-effective but could benefit the American economy by up to $25.99 billion annually.” Massage therapy is an effective and cost-efficient pain management approach. Encouraging medical practitioners to prescribe its use in cases where it would be an effective pain management tool and insurance companies to cover massage therapy can significantly impact the opioid problem in the U.S. and decrease the costs associated with opioids and pain relief. [17]
Massage Therapy is Cost Effective for Pain Management
In the study entitled, Analysis of Provider Specialties in the Treatment of Patients with Clinically Diagnosed Back and Joint Problems (Wilson FA, et al), researchers looked at the cost-effectiveness of improving patient outcomes in patients with back and joint pain. In this study, researchers collected data from specific treatment providers: doctors (internal medicine, family/general, osteopathic medicine, orthopedics, rheumatology, neurology) or other providers (chiropractor, physical therapist, acupuncturist, massage therapist).
“Cost-effectiveness analysis suggests that osteopathic, family/general, internal medicine doctors and chiropractors and massage therapists were more cost-effective than other specialties in improving physical function to back pain patients,” the study found. The study further noted, “However, only massage therapy was cost-effective among non-doctor providers in improving quality of life measures.” [18] Figure 12.
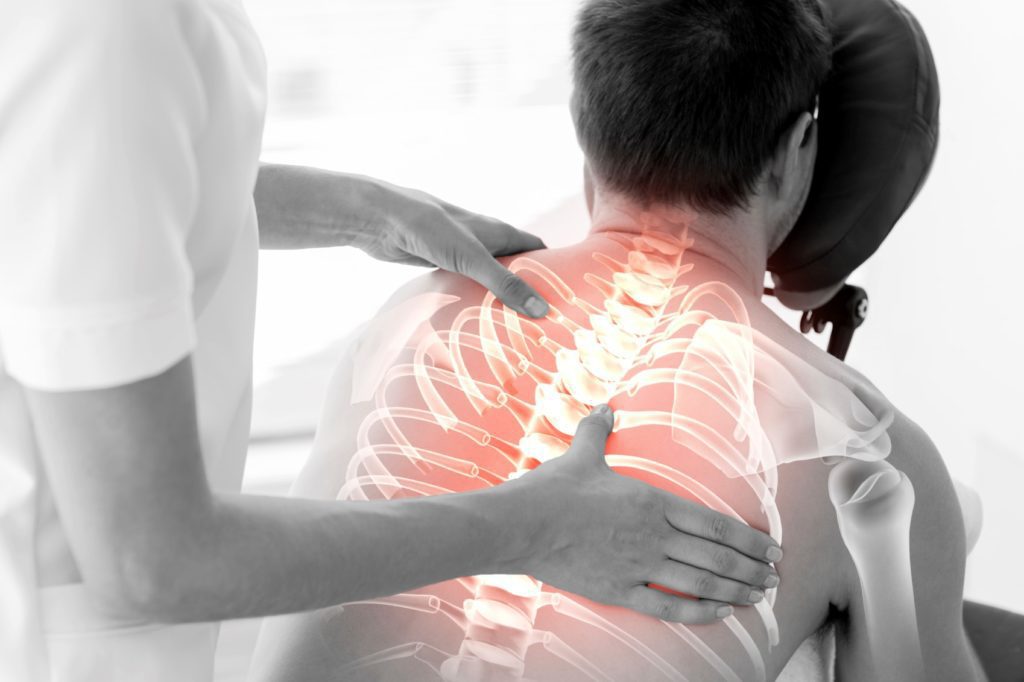
Figure 12: Massage therapy in back pain
Yoga and Meditation as cost effective treatment
A new research study shows that a little yoga or meditation a day might just keep the doctor away.
Stress-related health problems are responsible for up to 80% of visits to the doctor and account for the third highest health care expenditures, behind only heart disease and cancer. But as few as 3% of doctors actually talk to patients about how to reduce stress.
Mind-body practices like yoga and meditation have been shown to reduce your body’s stress response by strengthening your relaxation response and lowering stress hormones like cortisol. Yoga has been shown to have many health benefits, including improving heart health and helping relieve depression and anxiety. Figure 13.

Figure 13: Yoga
Dr. James E. Stahl and his team of Harvard researchers studied a mind-body relaxation program offered through the Benson-Henry Institute for Mind Body Medicine at Massachusetts General Hospital. The 8-week program taught participants several different mind-body approaches, including meditation, yoga, mindfulness, cognitive behavioral skills, and positive psychology. The study volunteers participated in weekly sessions and practiced at home as well.
The researchers found that people in the relaxation program used 43% fewer medical (health and human) services than they did the previous year, saving on average $2,360 per person in emergency room visits alone. This means that such yoga and meditation programs could translate into health care savings of anywhere from $640 to as much as $25,500 per patient each year.
A recent article in the Harvard Business Review recommends that health insurers cover wellness and prevention-oriented therapies that are both low-cost and evidence-based, as both yoga and meditation are. The article discusses a study of Aetna employees who participated in the company’s mindfulness program and enjoyed a 28% reduction in stress, 20% better sleep, and 19% less pain, as well as an increase in worker productivity worth an estimated $3,000 per employee per year. The company offers free yoga and meditation programs to its employees. [19]
Yoga and Meditation for Stress and Depression
Yoga and meditation can be great ways to relax and quiet the mind, and a growing body of research has shown that these mindfulness practices may even be effective for treating physical and mental health problems ranging from heart disease to depression.
Mind-body practices may also keep you away from the hospital, according to a study by researchers at Benson-Henry Institute for Mind Body Medicine at Massachusetts General Hospital, and recently published in the journal PLOS One. Yoga and meditation, which trigger the body’s relaxation response and lower levels of the stress hormone cortisol, seem to prevent hospital visits due to stress-related health problems, which account for between 75 and 90 percent of all doctor’s visits. Figure 14.

Figure 14: Yoga in Stress management
More research is needed to confirm these results and demonstrate this effect in other settings. But for now, the findings offer reason to be optimistic about mindfulness as a low-cost, low-risk intervention for improving individual health and reducing public spending on health care.
“Mind-body medicine interventions are inexpensive relative to the cost of an emergency room visit, a hospitalization or even other complementary and alternative medicine therapies,” the study’s authors wrote, estimating overall annual savings –taking into account the costs of hospital and doctor visits, and medical tests — of up to $25,000 per patient. [20]
Health Insurance Companies Coverage for Yoga
Some health insurers already cover many forms of complementary health therapies, such as acupuncture and massage. Plus, health insurers often reimburse gym memberships or partner with fitness programs to provide a discount, so it’s worth asking your individual insurance company. But most health insurers do not cover yoga, so we end up paying out-of-pocket.
The Affordable Care Act (ACA) aims to cover preventative medicine and wellness-based treatment but does not specify coverage of complementary health therapies like yoga. As a result, coverage of complementary health treatment currently varies based on state and individual plans. A handful of states require coverage of complementary health care. Since 1996, Washington state law has required coverage of licensed complementary and alternative medicine providers. In 2014, acupuncture became an “essential health benefit” and covered under the Affordable Care Act in California.
Yoga for Stress Management in US
Stress is one of the top three health care costs in the U.S., behind only heart disease and cancer. Stress-related problems account for up to 80-90% of visits to the doctor, but only 3% of doctors talk about how to reduce stress with their patients.
A recent study conducted by Dr. James E. Stahl and his team at Harvard-affiliated Massachusetts General Hospital found that people who participated in an 8-week yoga and meditation program used 43% fewer medical services than the previous year, saving on average $2,360 per person in emergency room visits alone. This means that such yoga and meditation programs could translate into health care savings of $640 to $25,500 per patient each year.
Health care consultants have also recommended that health insurers cover wellness and prevention-based therapies like yoga in a recent article in the Harvard Business Review. Aetna, under the leadership of chairman and CEO Mark T. Bertolini, offers free yoga and meditation programs for Aetna employees. A study of Aetna employees who participated in the company’s mindfulness program found a 28% reduction in stress, 20% better sleep, and 19% less pain. This translated into increased worker productivity worth an estimated $3000 per employee per year. [21]
SATYAM-“Science and Technology of Yoga and Meditation” inspiring Cheap Alternative Therapy:
A new program called SATYAM-“Science and Technology of Yoga and Meditation” has been launched to strengthen research in the areas of yoga and meditation. An objective of SATYAM is to harness knowledge obtained in academic institutions and other related agencies for finding Science & Technology -led solutions that would enable us to cope with stress and strain associated with fast-changing social, economic, environmental, and professional circumstances. Cutting-edge research under SATYAM will seek to identify various issues and challenges related to human well-being and address them. The program will encourage research in two major thematic areas:
- investigations on the effect of Yoga and meditation on physical and mental health
- Investigations on the effect of Yoga & meditation on the body, brain and mind in terms of basic processes occurring therein.
Given the ever-increasing prevalence of physical and mental health problems, the holistic approach of Yoga and meditation is believed to have the potential to find beneficial treatment that is relatively safer and more cost-effective. [22]
Colon Hydrotherapy is Cost Effective and is not covered by Health Insurance
The colon is the large intestine, and it absorbs water and salts from waste material that has traveled through the body. Bacteria in the colon break down the remaining material, which then exits the body through the rectum and anus. Some people believe that hydrotherapy can cleanse the colon, and the Association of Registered Colon Hydrotherapists (ARCH) refers to the procedure as simple, safe, and convenient. However, scientific evidence does not support colonic hydrotherapy as a way to cleanse the body or improve health. Figure 15.

Figure 15: Colon Hydrotherapy
Some practitioners claim that colonic irrigation helps treat symptoms of irritable bowel syndrome (IBS). This is based partly on a 2016 study that included only 18 participants, who reported improved IBS symptoms after colonic irrigation. Among the improved symptoms were abdominal pain, constipation, and diarrhea, and the participants also reported feeling more satisfied with their bowel movements and less disturbed by their symptoms.
It is important to highlight, however, that this study was very small and included no control group. The researchers acknowledge the need for further studies including placebos and larger studies that investigate the long-term effects, including those on the quality of life. Health insurance does not cover hydrotherapy of the colon because it is an elective procedure. Prices vary, depending on location, but each session is likely to cost at least $45. [23]
According to the Colon Therapists Network, prices for colon irrigation range between $55 to $95 per treatment, varying between locations and centers. Depending on the facility, packages and discounts can increase the affordability of this treatment since it is not traditionally covered by medical insurance.
Because this therapy is considered a form of alternative medicine, most insurance policies will not cover or discount the cost. However, it can be more affordable by making payments through a heath flex spending account. This type of account allows individuals to set aside part of their paycheck tax-free to cover health-related expenses. [24]
Mud Therapy is Cost Effective

Earth is one among five elements having an immense impact on human body. It has been adopted as a treatment modality, i.e., mud therapy in naturopathy. It is a simple, cost effective and efficacious treatment used in the treatment of various disorders. Mud is used as a medicine since long as various references are found available in ancient texts indicating its therapeutic uses. Mud has various therapeutic properties which are highly useful in the treatment of various disease conditions. The paper highlights the therapeutic uses of mud as a therapy and its importance, possible role and usefulness in the modern times. [25] Figure 16.
Figure 16: Mud therapy is cost effective
Naturopathy Offers Cheap Treatment for Infertility
All the naturopathic medicines are nontoxic and that is why they are safer than any other type of traditional and modern treatments. Some of the traditional medications and treatments may have stern side effects. For instance, traditional medicines for ovary stimulation can over stimulate them to cause severe pain that may even need hospitalization. Naturopathic medicines on the other hand have no adverse side effects.
Since naturopathy is based on healthy nutrition and lifestyle, it is quite apparent that while treating infertility, the patient gets benefited with improved overall health as a result of healthy food choices. For example, through herbal treatments given to improve the egg or sperm quality, the overall immune system also gains strength and hormonal levels are balanced to enhance mood and functionality. Figure 17.

Figure 17: Treatment of infertility
If cost is one of the major factors to decide on which type of treatment to choose, naturopathic medicine is often far less expensive than conventional medications and treatments. However, the cost of naturopathic infertility treatment can vary according to the severity of the condition, but it is still a cost-effective option. Through naturopathic medicine, the entire fertility mechanism is treated to increase conception rates and maintain a healthy pregnancy.
Acupuncture in Pregnancy
Acupuncture has been studied in many ways with respect to fertility. Here is a brief summary of the research findings:
- Acupuncture can increase rates of pregnancy in those undergoing IVF
- Acupuncture can enhance sperm quality and quantity
- Acupuncture can increase blood flow to the pelvis, thus improving ovarian function
- Acupuncture can help to regulate the menstrual cycle
- Acupuncture can help increase the thickness of the uterine lining (endometrium) Figure 18.

Figure 18: Acupuncture in Pregnancy
Researchers claim that naturopathic medicine uses the healing power of nature to maintain and restore health. Their goal is to create a healthy environment inside and outside the body. Naturopathic medicine prevents illness because people are taught healthy diets and lifestyles to avoid disease. Treatment is focused on the cause of disease, rather than on the symptoms. Naturopathic doctors may diagnose illness with many of the same methods used in conventional medicine. They use x-rays, laboratory tests, and physical exams to try to identify the problem. However, naturopathic treatment does not generally use drugs, radiation therapy, or major surgery which are actually too much costly tests and treatments as well.
Naturopathic medicine is promoted for the treatment of conditions such as migraine headaches, chronic lower back pain, enlarged prostate, menopause, AIDS, and cancer. Practitioners claim to use “natural methods” to strengthen the body’s ability to heal itself. They believe that this type of care causes fewer side effects and costs less than conventional treatment. However, practitioners often refer complicated cases or people needing major treatment to conventional medical professionals.
References
- https://worldpopulationreview.com/country-rankings/medical-bankruptcies-by-country
- https://www.cnbc.com/2019/02/11/this-is-the-real-reason-most-americans-file-for-bankruptcy.html
- https://www.forbes.com/advisor/debt-relief/medical-bankruptcies/
- David U. Himmelstein, et al. “Medical Bankruptcy in the United States, 2007: Results of a National Study,” Page 741. Elsevier Inc, 2009.
- Himmelstein, D. U., Lawless, R. M., Thorne, D., Foohey, P., &Woolhandler, S. (2019). Medical bankruptcy: still common despite the Affordable Care Act. American Journal of Public Health, 109(3), 431-433.
- Kaiser Family Foundation. “Kaiser Family Foundation/LA Times Survey of Adults With Employer-Sponsored Health Insurance,” Page 10.
- https://www.theguardian.com/us-news/2019/nov/14/health-insurance-medical-bankruptcy-debt
- Amadeo, K. (2018). Medical bankruptcy and the economy.
- https://www.survivorshipatoz.org/breastcancer/articles/naturopathy/?sid=2754
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6476478/
- Willich, Stefan N.*; Reinhold, Thomas; Selim, Dagmar; Jena, Susanne; Brinkhaus, Benno; Witt, Claudia M.. Cost-effectiveness of acupuncture treatment in patients with chronic neck pain. Pain: November 2006 – Volume 125 – Issue 1 – p 107-113 doi: 10.1016/j.pain.2006.06.006
- Shuji Ono, Yoshito Mukaino, “Efficacy and Cost Effectiveness of the Acupuncture Treatment Using a New Skin Stimulus Tool Called M-Test Which Is a Measure Based on Symptoms Accompanied with Body Movements: A Pragmatic RCT Targeting Hemodialysis Patients”, Evidence-Based Complementary and Alternative Medicine, vol. 2015, Article ID 802846, 8 pages, 2015. https://doi.org/10.1155/2015/802846
- Stamuli, E., Bloor, K., MacPherson, H. et al. Cost-effectiveness of acupuncture for irritable bowel syndrome: findings from an economic evaluation conducted alongside a pragmatic randomised controlled trial in primary care. BMC Gastroenterol 12, 149 (2012). https://doi.org/10.1186/1471-230X-12-149
- CCRH Research Policy. Central Council for Research in Homeopathy, Ministry of Health and Family Welfare; Government of India. Available at: https://ccrhindia.org/imrpolicy.pdf Accessed 15.12.14. [Ref list]
- Tripathy JP. Can naturopathy provide answers to the escalating health care costs in India? J Tradit Complement Med. 2015 Jan 16;5(2):63-5. doi: 10.1016/j.jtcme.2014.11.006. PMID: 26151012; PMCID: PMC4488104.
- Center for Medicare & Medicaid Service, DRG Summary for Medicare Inpatient Prospective Payment Hospitals, FY2015, August 30, 2017, Online at: https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Medicare-Provider-Charge-Data/Inpatient2015.html and Center for Medicare & Medicaid Service, APC Summary for Medicare Outpatient Prospective Payment System Hospitals, CY2015, August 30, 2017. https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Medicare-Provider-Charge-Data/Outpatient2015.html
- https://www.prnewswire.com/news-releases/massage-therapy-can-reduce-the-cost-of-the-national-opioid-crisis-300731276.html
- https://www.massagetherapycanada.com/study-shows-massage-therapy-is-cost-effective-3028/
- https://www.health.harvard.edu/blog/yoga-and-meditation-offer-health-care-savings-and-you-can-do-them-at-home-201511188616
- https://www.huffpost.com/entry/yoga-meditation-health-care-costs-study_n_562fa500e4b06317990f8754
- https://www.psychologytoday.com/intl/blog/urban-survival/201511/who-should-help-pay-yoga
- https://pib.gov.in/newsite/PrintRelease.aspx?relid=130289
- https://www.medicalnewstoday.com/articles/hydrotherapy-of-the-colon#procedure
- https://www.leaf.tv/articles/how-much-does-colonic-hydrotherapy-cost/
- https://www.researchgate.net/publication/289594861_Therapeutic_uses_of_Mud_therapy_in_Naturopathy
- Grace, Sandra, et al. “The Cost-Effectiveness of Natural Medicine: An literature review.” Journal of the Australian Traditional-Medicine Society, vol. 24, no. 1, autumn 2018, pp. 14+.GaleAcademicOneFile,link.gale.com/apps/doc/A546447507/AONE?u=anon~9b15bad9&sid=googleScholar&xid=2a5a332c. Accessed 10 Sept. 2022.
